Do you know the secrets about the human liver anatomy? Which is the hottest internal organs with incredible regenerative capacity? What if 75% of the organ is lost in a disease?
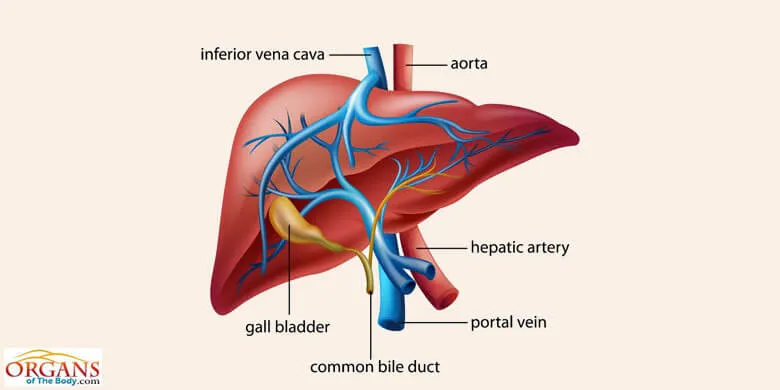
Fig. 1: Human Liver
What is liver definition? Sitting to the left of the belly, liver is the largest internal organ that supports almost every other organ in your body. It has a reddish-brown appearance and feels rubbery to the touch. This vital organ is responsible for hundreds of chemical reactions that are necessary for your survival.
Table of Contents
- The Human Liver Size
- Liver Location
- The Human Liver Anatomy
- Liver Function
- Liver as a Filter
- Processing Nutrients
- Blood Reservoir
- Synthesis and Storage of Glycogen
- Conversion of Glycogen to Glucose
- Restoration of Glucose Level
- Glucose from Non-Carbohydrate Compound
- Synthesis of Blood Clotting Factors & Other Plasma Proteins
- Synthesis of Glycoproteins, Enzymes, etc.
- Detoxification of Poisons and Drugs
- Conversion of Ammonia to Urea
- Lipid Metabolism
- Alcohol Metabolism
- Synthesis of Bile
- Storage of Vitamins and Iron
- Storage of Minerals
- Destruction of Old RBCs
- Liver Function Test
- Regenerative Capacity of Liver
- Signs of Liver Disease
- Risk Factors for Liver Disease
- Types of Liver Diseases
- Causes of Acute and Chronic Liver Diseases
- Liver Transplant
- References
The chemical factory of your body, liver works tirelessly 24/7 and performs over 500 function vital to your life.
As a gland, liver secretes bile which is emptied into the small intestine to facilitate digestion.
Skin is the largest organ, whereas liver is the largest internal organ and the largest gland in the human body.
Precisely, it is one of the most fantastic organs of your body.
Here, you will get useful and interesting information about the liver size, location, function, diseases and risk factors for liver disease.
The Human Liver Size
Different factors, like age, gender and body size, affect the liver size. It is bigger in human males than that in females. The size of this gland is around 10.5 centimeters for men and about 7 centimeters for women. In the similar way, the liver weight is also different in different genders. Normal liver weighs about 1.2 to 1.5 kg in females and males, respectively.
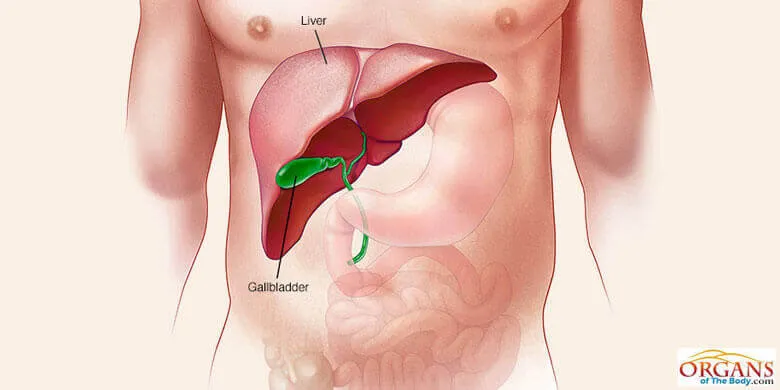
Fig. 2: Human Liver Size
Liver Location
The largest internal organ, liver appears in the right upper quadrant of the abdomen. It lies just beneath the right side of the diaphragm and under the right lower rib cage. Concerning human liver anatomy, there are eight functional segments in it.
Within a minute, approximately 1500 ml of blood flows through the liver. This is so to ensure its efficient working. Partly due to its ample blood supply, liver is the prime site for metastatic spread of cancer.
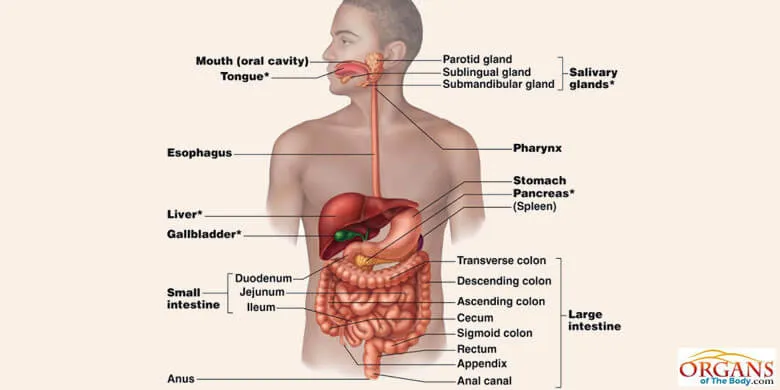
Fig. 3: Location of Liver in Human Body
Read Further: Where is Liver Located in female body?
The Human Liver Anatomy
The human liver anatomy is easy to understand. When you view the organ from above, it seems to contain two lobes. On the other hand, viewing it from underside, reveals that there are four lobes of the liver. From the above view, the left lobe is smaller than the right one.
Going deeper into the human liver anatomy, you will find that both the lobes consist of 8 segments. These segments contain nearly 100,000 lobules.
A thin double-layered membrane makes a covering around it. You call this covering the peritoneum. It is this peritoneum which minimizes friction of the liver against other organs.
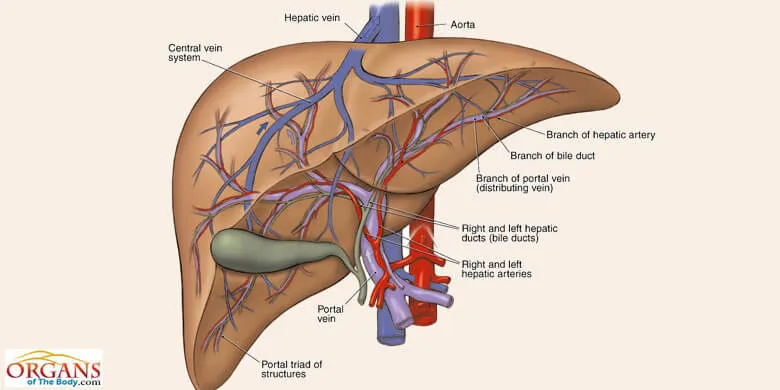
Fig. 4: Human Liver Anatomy
Types of Liver Diseases
In this article, you will find a list of liver diseases of various kinds. But, it is not the exhaustive list. Here you will also learn about the liver disease symptoms, tests, causes and remedies.
Jaundice
Jaundice is one of the common types of liver diseases that refers to the golden yellow appearance of skin and sclera. It results from too much accumulation of bilirubin in the body fluids. Jaundice is first noticeable in the sclera of the eyes. You call this yellow discoloration of the sclera as icterus. Jaundice is evident in skin when serum bilirubin level is 2.5 to 3 mg/dL.
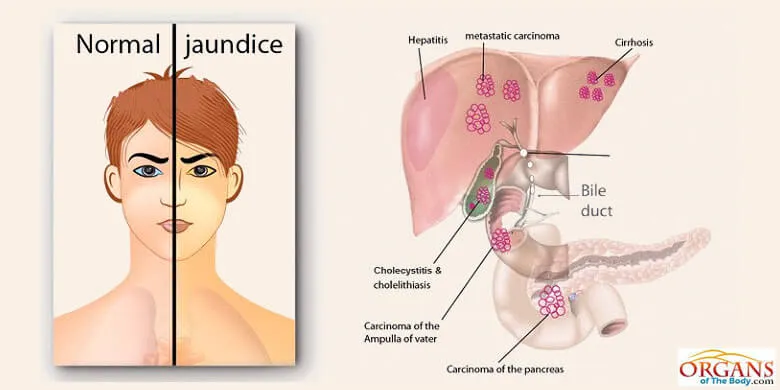
Fig. 11: Jaundice
Causes of Jaundice
- Overproduction of bilirubin.
- Less hepatic uptake of bilirubin
- Impaired conjugation of bilirubin
- Defective hepatocellular excretion of bilirubin
Symptoms of Jaundice
- The most significant symptom is the yellowing of the skin and the sclera, the white part of your eyes.
- Abdominal pain which is characteristic of the blockage in the bile duct.
- Other symptoms include fever, fatigue, vomiting and the weight loss, etc.
Treatment of Jaundice
The hike in bilirubin level is actually due to the rapid breakdown of red blood cells. This occurs due to some disease and infection that also affects liver. So, the treatment of jaundice completely depends on the cure of underlying cause. In other words, you have to identify and treat the condition that is responsible for the higher level of bilirubin in the body.
Drug-induced Hepatotoxicity
As the very name implies, drug-induced hepatotoxicity is one of the types of liver diseases which occur due to the effect of drugs on liver. Many drugs can harm the liver severely. Therefore, it is always wiser to consult a health professional before taking any medicine. And you should refrain from self-medication.
Fig. 12: Drug-induced Hepatotoxicity
Causes of Drug-Induced Hepatotoxicity
Here are some of the harmful drugs which lead to different types of liver diseases:
- Acetaminophen – The drug can cause necrosis or injury and death of the hepatocytes, the liver cells.
- Oral Contraceptives – Hepatic adenoma may result from the harmful effects of oral contraceptives.
- Halothane – The use of halothane puts the individuals at the risk of developing fulminant hepatitis.
- Sulfonamides – With the intake of sulfonamides, you may fall victim to granulomatous. Thus, the phagocytes are unable to kill some types of fungi and the bacterial species.
- Phenytoin, Isoniazid – These drugs can lead to the development of acute and chronic hepatitis.
- Methotrexate, Amiodarone – Different types of liver diseases, like fibrosis and cirrhosis may result from the use of methotrexate and amiodarone, etc.
- Chlorpromazine – If you take chlorpromazine, you would be at the risk of cholestasis.
Alcoholic liver disease
The overuse of alcohol can cause several types of liver diseases. They include the buildup of fat in the liver, alcoholic cirrhosis, alcoholic hepatitis, and so on. In comparison with men, women seem to be more susceptible to alcoholic liver injury.
Alcoholic cirrhosis which develops in 15% of the alcoholics is the most common disease that requires liver transplantation in adults.
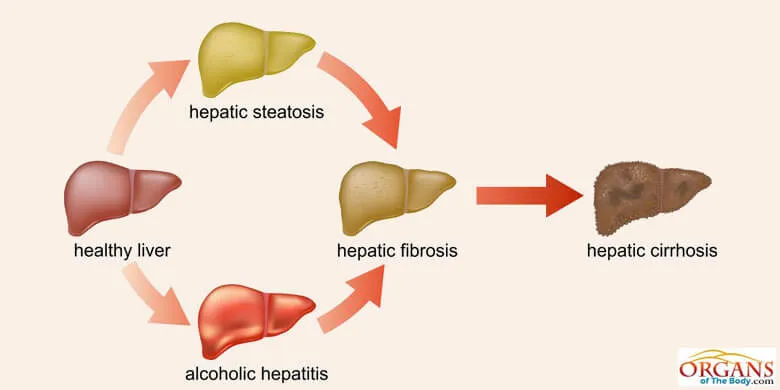
Fig. 13: Alcoholic Liver Disease
Symptoms of Alcoholic Liver Disease
As a result of the alcoholic liver disease, the patient may develop following symptoms:
- Loss of appetite followed by the weight loss.
- Fatigue due to the lack of energy, and it can be debilitating.
- Appearance of the characteristic symptoms of the jaundice, for example, yellowing of the skin and sclera.
- Retention of fluid and inflammation in legs, ankles and the abdominal region, etc.
Treatment of Alcoholic Live Disease
The first step towards the treatment of this condition is to abstain from alcohol. However, the suggestion of a particular treatment strategy depends on the specific type of alcohol-related liver disorder.
Nevertheless, in all such conditions, the cessation of alcohol is essential. In this way, you can prevent the liver from further damage. On the other hand, the use of medication will help liver synthesize its damaged cells.
Cirrhosis
Cirrhosis is an end-stage liver disease. Here alcohol is the direct hepatotoxin. And it is the most common cause of cirrhosis in the western world. In cirrhosis, there is total disruption of the liver architecture due to fibrosis and nodule formation.
This disruption in the liver architecture eventually interferes with liver blood flow and function.
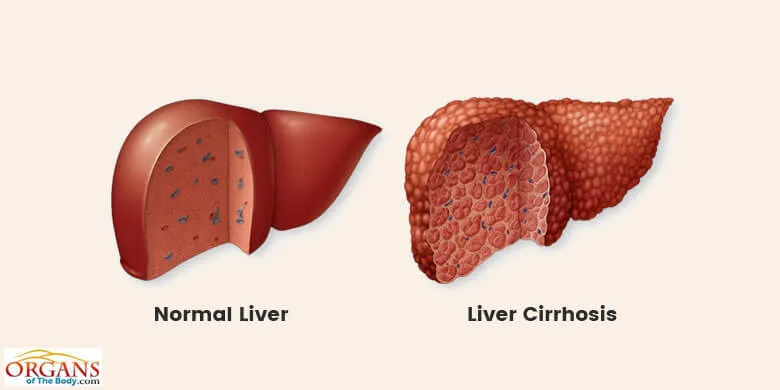
Fig. 14: Cirrhosis Liver
Cirrhosis Causes
- Too much consumption of alcoholic beverages.
- Blockage in the bile duct which may be due to some other liver disease.
- Buildup of fats in the organ.
- Chronic viral infections, for example, hepatitis B and C.
Cirrhosis Treatment
Usually, no medication can reverse the damage that has occurred to the liver due to cirrhosis. However, certain medicines can stop further damage to the organ. In this regard, the changes in lifestyle will also be helpful.
Nevertheless, the best treatment option is to go for the liver transplant. It will restore the normal function of the organ.
Other Liver Diseases
- Hepatitis A, B, C, D, E – These are different types of liver diseases that occur by the at-tack of different types of viruses. For example, hepatitis A occurs due to hepatitis A virus, and the causative agent for hepatitis B is the hepatitis B virus.
- Fulminant Hepatic Failure (FHF) – FHF is the condition of acute liver failure which se-verely impairs synthetic function of the organ.
- Drug-induced Chronic Hepatitis – Excessive use of drugs causes inflammation of liver which may last for six months or more.
- Non-alcoholic Fatty Liver Disease – When there is the storage of too much fat in the liver, it leads to non-alcoholic fatty liver disease in the people who consume little to no al-cohol.
- Budd-Chiari Syndrome (BCS) – BCS is a rare liver condition which results from the obstruction in the hepatic veins.
- Fibropolycystic Liver Diseases – In this group of congenital disorders, there is the for-mation of lesions in the liver and the bile ducts. Here the causative agent is the abnormal embryologic development of the ductal plates.
- Hepatic Sinusoidal Obstruction Syndrome – The exposure to toxins and drugs is the major contributing factor towards the development of this fatal form of hepatic injury.
- Liver Abscess – The abdominal infections, like appendicitis and diverticulitis, trigger the formation of pus-filled mass inside the organ.
- Liver Tumors – The benign or noncancerous liver tumors, usually, do not pose a serious risk for health. The malignant or cancerous liver tumors, on the other hand, pose a seri-ous health risk. They can be either primary or metastatic. The first type, the primary he-patic tumors originate in the liver.
- In the second type, the metastatic liver tumor, the cancer develops elsewhere in the body and spreads to the liver.
- Wilson's Disease – The Wilson’s disease is a rare type of the recessive autosomal con-genital disease. In this case, there is an abnormal copper metabolism in the body. Con-sequently, there is the accumulation of copper especially in the liver and the brain. If you do not treat it timely, the condition can also claim the life of the victim.
- Hemochromatosis – In this genetic disorder, there is excessive accumulation of iron in the organs, like liver. On the other hand, too much amount of iron leads to liver toxicity.
It was a list of liver diseases of several kinds. A healthy diet can save you from all such disorders.
Causes of Acute and Chronic Liver Diseases
The most common causes of acute liver disease (severe and sudden in onset) are:
- Viral Hepatitis – Viral infection of liver occurs due to the attack of hepatitis B or C virus, etc.
- Drug-induced Liver Injury – In this type of injury, drugs cause a damage to the liver.
- Cholangitis (Inflammation of Bile Duct) – There is blockage in the bile duct which leads to its swelling.
- Alcohol Abuse – Consuming too much alcohol is injurious to the health of liver. The al-cohol addict is likely to fall victim to several types of liver diseases.
The most common causes of chronic liver disease (long developing syndrome) are:
- Chronic Hepatitis C – The chronic hepatitis C serves as one of the major causes for the chronic liver disease.
- Alcohol Abuse – Alcoholism can be the cause of both acute and chronic hepatic disor-ders.
- Nonalcoholic Steatohepatitis – When hepatitis does not occur due to alcohol abuse, it is called nonalcoholic steatohepatitis.
- Chronic Hepatitis B – This viral infection results in the scaring, failure and cancer of the liver.
- Autoimmune Hepatitis – In the autoimmune hepatitis, the immune system attacks and damages the liver cells and components.
- Sclerosing Cholangitis – The chronic liver condition of sclerosing cholangitis involves the swelling and fibrosis of the bile ducts.
- Primary Biliary Cirrhosis – This autoimmune disorder causes slow destruction of the small bile ducts.
- Hemochromatosis – As the name indicates, it involves excessive accumulation of iron in the organ.
- Wilson's Disease – The Wilson’s disease is the result of excessive copper accumulation in the organ.
Liver Transplant
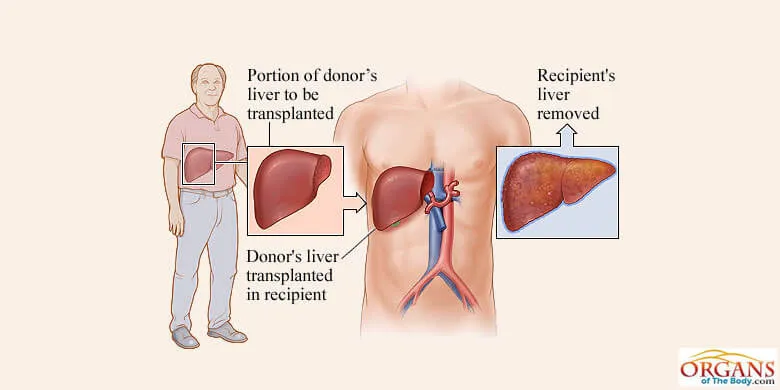
Fig. 15: Liver Transplant
The transplant is the only choice for patients with end-stage liver disease. Surgical therapy is used to replace a diseased and damaged liver with a normal organ. It is because chronic or acute liver disease is progressive, life threatening and unresponsive to medical therapy.
After the transplantation, for low risk patients, current level of success or survival rate is approximately 90% for one year and 60% for five years.
But, for high risk patients especially those suffering from cancer, fulminant hepatitis, and having age more than 65, the success rate is different. The current survival rate for them is approximately 60% for one year and 35% for five years.
References
- Healthline, Liver
- WebMD, Picture of the Liver, Prothrombin Time
- Stanford Children’s Health, Anatomy and Function of the Liver
- British Liver Trust, Liver Health
- Wolf, D. C. (1990), Evaluation of the Size, Shape, and Consistency of the Liver. Clinical Methods: The History, Physical, and Laboratory Examinations (3rd ed., Chapter 94). Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK421/
- Openstax CNX, Accessory Organs in Digestion: The Liver, Pancreas and Digestion
- Wikipedia the Free Encyclopedia, Liver, Alanine Transaminase
- Lab Tests Online, Bilirubin
- Medline Plus, Bilirubin – Urin, Albumin Blood Serum Test
- American Liver Foundation, Liver Function Tests
- The Johns Hopkins Complete Guide to Symptoms and Remedies (2004), published by Black Dog & Leventhal Publishers, Inc.


