Kidney Function - The Kidneys Function in Excretory & Endocrine System
What is Kidney Function?
The primary kidney function is to purify the blood by removing waste and harmful substances. The structural and functional unit of the kidney is called the nephron. Each human kidney contains more than 1 million nephrons. It is with the help of nephrons that kidneys remove metabolic waste products from the body. Another important kidney function is to regulate fluid and electrolytes balance within the body.
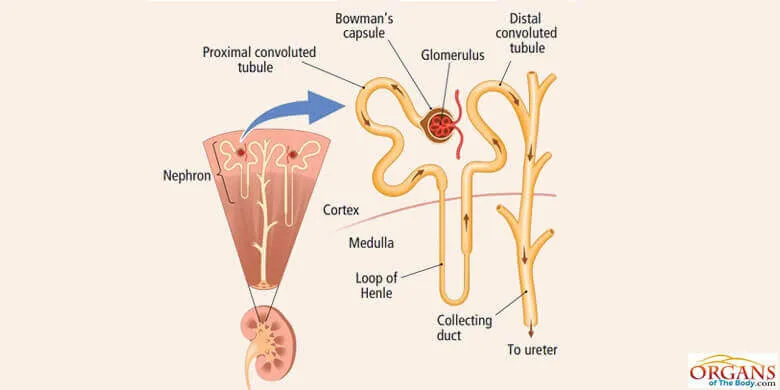
Nephron – Basic Unit of Kidney Function:
is parallel alignment of nephrons to perform the kidney function of purifying blood. Each individual nephron functions almost exactly the same as all other nephrons in both of the kidneys. If you clearly understand how one nephron works you would readily understand nearly everything about how the kidneys execute their functions successfully.
Types of Nephrons:
Depending on the location of the renal corpuscle there are two types of nephrons, i.e. cortical nephrons and juxtamedullary nephrons. Of these, 85% are cortical nephrons and the rest are juxtamedullary nephrons. Cortical nephrons have short loop of Henle while juxtamedullary nephrons have long loop of Henle.
Functional Segments of a Nephron:
A nephron has various functional segments. Each segment has to perform specific biological functions essential to maintain biochemical homeostasis (stable internal environment) within a narrow range.
Each nephron has several distinct parts. These are: renal corpuscle, proximal convoluted tubule, loop of Henle, distal convoluted tubule and collecting duct. Renal corpuscle is the initial dilated portion of the nephron. It consists of glomerulus and Bowman's capsule.
Blood passes from the glomerulus into the Bowman's capsule and then enters the proximal convoluted tubule. From here it goes into the long loop of Henle. Finally, the blood enters the distal convoluted tubule and collecting duct.
From the collecting duct, the ultra-filtrate of the blood flows into the renal pelvis. Here the renal pelvis is actually a funnel shaped expansion of the upper end of the ureter. Ureter carries the final product (urine) from the renal pelvis of each kidney to the urinary bladder.
At the point of bladder, there is temporary storage of urine. The urine stays here till the time you discharge it out of the body through urethra.
Renal Corpuscle (Glomerulus & Bowman’s Capsule):
Glomerulus is basically a tuft of small capillaries. Glomerulus primarily filters the blood plasma. Whereas, the tubular parts of the nephron convert the filtrate into urine. The blood that enters the glomerulus is gradually modified as it flows along the various parts of the nephron.
During the process of modification, there is reabsorption of most of the water and electrolytes into the blood. But almost all of the metabolic end products become part of the urine. Initial glomerular filtrate has biochemical constituents similar to that of the blood plasma.
The glomerular filtrate contains very minute amount of macromolecules such as albumin. It is because proteins or any particles greater than 10 nm in size do not readily cross the glomerular filtration barrier. However, the same may occur in diseases like diabetes mellitus and inflammation of the glomerulus.
Presence of large proteins in the urine indicates many potential kidney disorders. Glomerular filtration barrier (GFB) is a negatively charged barrier. So it automatically repels substances or molecules that have negative charge (e.g. plasma proteins) except the ions.
GFB also restricts the passages of blood cells, platelets and leukocytes into the urine.
Proximal Convoluted Tubule:
It has got an important role to play in the overall kidney function. Tubular cells of the proximal convoluted tubule reabsorb several different useful substances. They include amino acids, vitamins, glucose, hormones, smaller plasma proteins, phosphate, ketones, calcium, large amount of sodium chloride. It also reabsorbs 65% of the water that was originally filtered in the renal corpuscle.
In addition, proximal convoluted tubule actively secretes creatinine, ammonia, hydrogen ions. Thereby, it helps the body get rid of foreign substances and drugs such as penicillin, morphine and salicylates.
Loop of Henle:
It is a U-shaped structure with a descending limb and an ascending limb. This part of the nephron principally performs the kidney function of water retention. In this way, it produces either concentrated or diluted urine and maintains extracellular fluid (ECF) homeostasis.
Meanwhile, there is reabsorption of a few ions such as bicarbonate, chloride, calcium, potassium, and sodium into the blood.
Distal Convoluted Tubule:
The maintenance of acid-base balance is also an important kidney function. In the distal convoluted tubule, the aldosterone hormone triggers the reabsorption of sodium and water. This part of the nephron plays the most significant role in maintaining the acid-base balance and total salt-water ratio of the body.
Collecting duct:
Finally, in the collecting ducts of the nephron, water is reabsorbed under the influence of another hormone, i.e. antidiuretic hormone (ADH). It occurs during dehydration or when the water ingestion is less. Depending on the dietary intake, there is either reabsorption or secretion of potassium in this part of the nephron.
The Kidney Function:
Apart from being an excretory organ, the kidney function also involves several other tasks. These include the maintenance of acid-base homeostasis, synthesis of glucose, regulation of different substances, and so on. Here follows a brief description of the major kidney functions:
Role in Excretion:
Kidney excretes harmful metabolic waste products, especially, nitrogenous compounds, such as urea, uric acid and creatinine. It helps the body in the removal of metabolites of various hormones and end products of hemoglobin breakdown. The kidneys also eliminate drugs, pesticides, food additives and other foreign toxic substances from the body.
Acid-base Homeostasis:
Kidney maintains the acid-base balance in the body. for this purpose, it controls the synthesis and excretion of bicarbonate and hydrogen ions. The organ can generate enough bicarbonate ions to neutralize net acid production from metabolism. All the renal tubules are capable of secreting a large amount of hydrogen ions into the urine eliminating excess hydrogen ions from the blood.
Glucose Synthesis:
Kidney reabsorbs essential nutrients such as amino acids from the filtered blood. During prolonged fasting kidneys can synthesize glucose from amino acids and then release glucose into the blood.
Calcium Homeostasis:
Here is another kidney function, i.e. it maintains calcium homeostasis by reabsorbing more than 90% of the filtered calcium. Reabsorption occurs in the proximal convoluted tubule and in the thick ascending limb of loop of Henle. Parathyroid hormone and vitamin D are the major hormones that influence calcium balance in the body. Parathyroid hormone acts on the distal convoluted tubule to increase calcium reabsorption into the blood.
Sodium and Water Metabolism:
As one of the important kidney functions, it regulates water balance within the body. For this purpose, either the kidneys concentrate or dilute the urine. Sodium reabsorption occurs along the entire length of the nephron to a varying degree.
Very little sodium becomes part of the urine. More than 67% reabsorption of the filtered sodium occurs in the proximal convoluted tubule. The pituitary gland releases antidiuretic hormone (ADH) when the sodium ion concentration becomes too high.
This causes kidney to retain more water. Greater quantity of water dilutes the excess sodium back to normal. There is also an increase in the blood volume. This, in turn, increases the arterial pressure in the kidney thus causing it to excrete more water and along with it excess sodium in the urine.
Regulation of Potassium, Phosphate and Magnesium Concentration:
High potassium ion concentration in the extracellular fluid (ECF) stimulates adrenal glands. They release aldosterone hormone. This hormone causes tubular cells in the kidneys to transport more potassium from the blood plasma and into the urine.
Majority of the filtered phosphate ions are reabsorbed in the proximal convoluted tubule by sodium-phosphate co-transporter.
The reabsorption of magnesium takes place in the proximal tubule, loop of Henle and in the distal tubule of the nephron.
Regulation of Blood Pressure and Volume:
When the volume of the blood becomes too high, blood pressure in the arteries increases. Such a condition increases the glomerular filtration. After that the kidney gets rid of excess water in the urine which returns the blood volume back to normal.
Kidney Function in Endocrine System
Release of Renin:
It is a hormone that the juxtaglomerular apparatus of the kidney produces. The production starts in response to low blood pressure in the renal arteriole. Renin then initiates a cascade of events that result in the production of angiotensin ll and aldosterone.
Angiotensin ll raises blood pressure by causing vasoconstriction and by raising total peripheral resistance. It also stimulates adrenal cortex to release aldosterone, resulting in higher sodium and water retention by the kidneys. This renin-angiotensin-aldosterone system accomplishes the long term regulation of blood pressure.
Production of Erythropoietin (EPO):
EPO is a glycoprotein hormone produced by the fibroblasts in the renal interstitium. Kidney is the main site of production of EPO. This hormone acts on the bone marrow to stimulate RBC (red blood cells) formation and maturation. If the patients with renal diseases do not get proper treatment, they will show profound anemia.
Activation of Vitamin D:
Hydroxylation of Vitamin D takes place with the help of an enzyme in the proximal convoluted tubule. Vitamin D in turn increases calcium and phosphorus absorptions from the gut. It also promotes bone mineralization.


